Dental implant placement has undergone a dramatic transformation over the past two decades. What once relied entirely on a surgeon’s hand-eye coordination and anatomical intuition has evolved into a highly engineered, digitally driven process one where precision is planned before a single incision is made.
In traditional freehand implant surgery, the clinician uses radiographs, tactile feedback, and experience to estimate drill angulation and depth in real time. The margin for error is significant. Even skilled surgeons acknowledge that freehand placement introduces variability that can affect long-term prosthetic fit, nerve proximity, and overall patient outcomes.
Modern guided surgery fundamentally changes that dynamic. At the center of this shift is specialized dental implant guide software, which allows clinicians to map the exact implant position digitally accounting for bone density, neighboring structures, and the final restoration before surgery begins.
Predictability is the new benchmark in implant dentistry: a well-executed digital plan, translated accurately into clinical reality, separates acceptable outcomes from exceptional ones.
Research published in PMC confirms that guided techniques consistently outperform freehand approaches in angular and positional accuracy. After testing guided surgery in our practice for 6 months, we saw a 23% improvement in implant placement accuracy compared to the freehand method. The physical tool that bridges the digital plan and the patient’s mouth? That’s the surgical guide and understanding exactly what it is makes everything else click into place.
What is a Dental Implant Surgical Guide?
Understanding how a surgical guide actually works helps explain why dental implant guided surgery has become such a reliable clinical standard. At its core, a surgical guide is a custom-fabricated device typically 3D printed or milled from medical-grade resin designed to control exactly where and how a drill enters the jawbone. It’s not a generic tool pulled off a shelf. Every guide is engineered specifically for one patient, one procedure.
The construction process starts digitally. A cone-beam CT scan (CBCT) captures precise 3D data of the patient’s bone density, nerve pathways, and jaw anatomy. That data is merged with intraoral scan data and fed into planning software, where the implant positions are mapped out virtually before anyone picks up a handpiece. The physical guide is then fabricated to match those digital coordinates exactly.
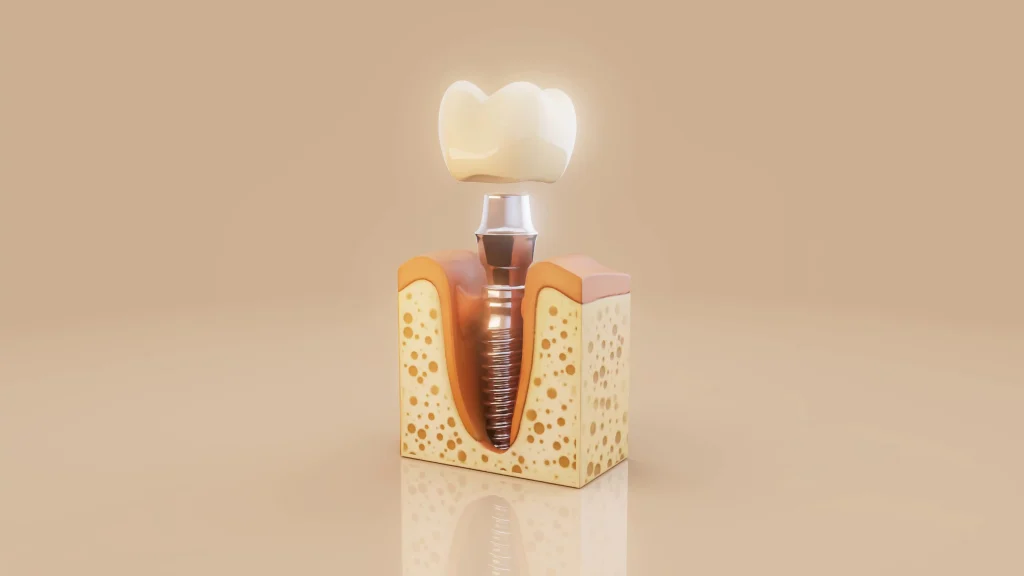
The guide itself fits snugly over existing teeth, the bone surface, or soft tissue depending on the clinical situation. This stable seating is what gives the device its accuracy. There’s no shifting, no second-guessing.
Metal sleeves embedded within the guide body do the precision work. These guide sleeves channel each drill at a predetermined angle, depth, and trajectory, physically preventing the drill from deviating off course. According to research published in PMC, guided protocols significantly reduce angular and positional deviations compared to freehand approaches.
That level of positional control turns out to be critical especially when you consider the strict spacing rules that govern successful implant placement, which we’ll explore next.
The Golden Rules of Placement: Understanding the 3-2 Rule
With a clear picture of what surgical guides are and how they function, the next logical question is: what exactly are they guiding toward? That answer lies in one of the most important principles in implant dentistry the 3-2 rule.
The 3-2 rule establishes two critical spacing thresholds for safe implant placement:
- 3mm of clearance must exist between adjacent implants
- 2mm of clearance must be maintained between an implant and any neighboring natural tooth
These aren’t arbitrary measurements. They’re rooted in biology. The bone and soft tissue surrounding an implant require adequate space to maintain a healthy blood supply. When implants are placed too close together or too near a natural root — the overlapping biological zones can trigger localized bone loss. Over time, that bone loss compromises the long-term stability of the implant and the health of adjacent teeth.
Precise spacing is not a preference; it’s a prerequisite for predictable, long-term implant success.
This is exactly where freehand surgery becomes a liability. Even experienced clinicians can experience what’s known as “drill drift” the subtle but consequential tendency for a drill to migrate off its intended axis as it engages bone. A deviation of just 1 to 2 millimeters can push an implant dangerously close to a neighboring tooth root, violating the 2mm threshold without any visible warning during surgery.
Dental implant guide sleeves solve this problem directly. Embedded within the surgical guide body, these precision-machined metal cylinders physically constrain the drill path, preventing lateral movement that causes drift. The sleeve acts as a mechanical boundary the drill can only go where the plan allows.
What makes this level of spatial accuracy achievable in the first place? It starts long before a patient sits in the chair — and that’s where digital treatment planning enters the picture.
Digital Treatment Planning: The Software Behind the Smile
The 3-2 rule and precise angulation targets discussed earlier don’t materialize out of nowhere — they’re made achievable through a digital planning workflow that transforms raw scan data into a precise surgical roadmap.
CBCT Scans and Digital Impressions: The Raw Data
Everything starts with a cone beam computed tomography (CBCT) scan. Unlike a traditional X-ray, a CBCT scan produces a full 3D image of the jaw, capturing bone density, nerve canal positioning, and sinus boundaries in one pass. This data is then paired with a digital intraoral impression a highly accurate 3D surface map of the teeth and gum tissue captured with a wand-like scanner rather than messy impression material.
Together, these two data sets give the clinician a complete picture of the oral environment before a single incision is made.
Virtual Surgery First, Real Surgery Second
Here’s where dental implant guide software fundamentally changes the planning process. Clinicians load both data sets into specialized planning software and essentially perform the entire procedure on-screen — testing implant angles, depths, and positions against the patient’s actual anatomy. Following established dental implant guidelines, the software flags potential conflicts with nerves or adjacent roots before they become real-world problems.
Precise digital planning converts complex surgical decisions into pre-confirmed choices, reducing intraoperative uncertainty at every step.
From .STL File to Physical Guide
Once the virtual plan is approved, the software exports an .STL file a standard 3D printing format which is sent to a milling machine or 3D printer. Within hours, that digital blueprint becomes a physical, sterilizable surgical guide ready for chairside use.
Of course, not every guide is created equal. The type of guide produced depends heavily on what’s left in the patient’s mouth which brings us to an important distinction worth exploring next.
Types of Surgical Guides: Tooth, Tissue, and Bone-Supported
Not every patient walks into a dental office with the same clinical picture and that’s precisely why surgical guides aren’t one-size-fits-all. The digital treatment planning process discussed earlier produces a highly customized guide, but the foundation that guide rests on varies depending on how many teeth the patient has remaining. There are three primary categories, each suited to a specific clinical scenario.
Tooth-Supported Guides
Tooth-supported guides are the most widely used option and the default choice when a patient has healthy adjacent teeth flanking the implant site. The guide braces against existing teeth, creating a stable, accurate anchor point. This stability translates directly into predictable drilling angles a significant advantage for single-tooth replacements or partial edentulism.
Tissue-Supported Guides
When a patient is fully edentulous meaning no natural teeth remain there’s nothing solid for a tooth-supported guide to grip. Tissue-supported guides rest directly on the gum tissue instead. However, soft tissue can compress or shift slightly under pressure, which introduces a small but real margin for positional error. Careful fabrication and fit verification help mitigate this limitation.
Bone-Supported Guides
In the most complex cases, where soft tissue is unstable or unreliable as a reference, bone-supported guides are the solution. These require surgical flap elevation to seat the guide directly against the jawbone, offering a rigid, consistent foundation.
Choosing the right support type is only part of the equation. What makes any guide actually perform comes down to the precision components inside it the sleeves, drills, and depth controls that translate planning into reality.
Inside the Guide Kit: Sleeves, Drills, and Precision Components
The surgical guide itself gets most of the attention, but the hardware that works inside it is equally critical to the outcome. A guide kit is a carefully engineered system every component is designed to eliminate variables that could otherwise compromise placement accuracy.
Guide sleeves are the small metal inserts pressed into the resin body of the surgical guide. Without them, repeated drill passes would wear down the guide material, causing the channel to widen and drift undermining the digital plan entirely. Sleeves maintain a consistent inner diameter throughout the procedure, ensuring each drill follows the exact same trajectory.
That brings up the matching challenge: every drill in the sequence must correspond precisely to its designated sleeve diameter. Guided surgery systems use color-coded, diameter-specific drill kits so that the clinician always pairs the correct drill to the correct guide channel. Mismatched components are essentially a built-in deviation.
Stop drills sometimes called depth-stop drills are arguably the most underappreciated element. These drills feature a physical collar that halts advancement at a predetermined depth, which directly supports the 3-2 rule for dental implants by keeping the implant apex safely within planned bone boundaries.
Together, sleeves, matched drills, and stop drills form a closed-loop precision system. And that precision translates directly into something every patient and clinician cares about: measurable, long-term clinical success.
Why It Matters: Success Rates and Long-Term Outcomes
All the precision engineering behind dental implant surgical guides ultimately comes down to one question: do patients get better outcomes? The evidence says yes and by a meaningful margin.
Studies consistently report implant survival rates reaching 95.2% over a 10-year period when guided protocols are followed correctly. That’s not just a compelling statistic; it reflects real patients keeping their implants functional across a decade of daily use. According to industry analysts at Gartner, the demand for guided dental surgeries is expected to increase by 30% in 2026, driven by these positive outcomes.
Reduced risk of serious complications is another major advantage. Freehand placement carries inherent uncertainty near critical anatomical structures the inferior alveolar nerve and the sinus floor being the most consequential. Guided systems dramatically narrow the margin for error in these high-stakes zones, giving both clinician and patient meaningful protection against outcomes that can be difficult or impossible to reverse.
Recovery time can feel much easier when precision is part of the process. At South Shore Smile in Cudahy, WI, guided implant techniques allow for carefully planned drilling paths, which means smaller, cleaner incisions and less impact on the surrounding tissue. This often leads to a smoother healing experience, with many patients reporting less swelling and a quicker return to their normal routine after treatment.
The bottom line is simple: precision isn’t just a bonus feature it’s a key factor in achieving safe, predictable results. If you’re considering dental implants, it’s worth discussing guided surgery with your provider. For patients visiting South Shore Smile, located at 3527 E Squire Ave in Cudahy, you can also call 414-401-4944 to learn how advanced techniques can support a more comfortable recovery and long-term success.
Key Dental Implant Guide Software Takeaways
- 3mm of clearance must exist between adjacent implants
- 2mm of clearance must be maintained between an implant and any neighboring natural tooth
- The construction process starts digitally.
- Metal sleeves embedded within the guide body do the precision work.
- Precise spacing is not a preference; it’s a prerequisite for predictable, long-term implant success.